Write Us
We are just a call away
[ LET’S TALK AI ]
X
Discover AI-
Powered Solutions
Get ready to explore cutting-edge AI technologies that can transform your workflow!


A healthcare team decides to build an AI app; the goal is to detect a rare disease early because patient data already exists inside the Electronic Health Record (EHR) system. The idea sounds simple, and it usually is explained that way. You take the patient data and you run it through an AI model and then you send the results back to clinicians so that decisions can be made faster but in real systems, the data does not sit in one place, rather, it is stored across tools that were never designed to work together and therefore the problem becomes less about AI and more about connection.
One system stores lab results, and another system stores clinical notes, but a third one manages patient engagement. And when these tools do not talk to each other properly, everything slows down. This is where SMART on FHIR app development starts to matter, because it was built for situations like this.
In many healthcare environments, information is still locked inside separate platforms and even though modern EHRs are already in place, interoperability is often fragmented. Teams have been building custom integrations for years but those connections are expensive and they are also difficult to maintain. This way of working no longer scales, and it creates more gaps than solutions because the demand for real-time clinical data has been growing.
SMART on FHIR provides a structured way for applications to connect with EHR systems by using FHIR APIs and secure OAuth 2.0 authorization so that developers do not need to rebuild the same integration again and again. Instead, a common standard is used, and because of that, data can move across systems with fewer disruptions, and for organizations involved in healthcare app development, this changes how clinical data is accessed, and how it is shared, and how it is used inside daily workflows.
There is also a shift that has been taking place at the platform level. What was once tested in pilot programs is now being moved into production environments. Hospitals, startups, and digital health companies are using SMART on FHIR integration for analytics tools, and for patient-facing apps and even for AI-driven decision support systems. Interoperability is no longer treated as a future goal, but rather as something that is expected now.
Today, we’ll discuss how to develop SMART on FHIR apps but before that, if you are planning a FHIR-based healthcare solution, or you are exploring how modern healthcare apps are built, it is therefore important for you to first understand how SMART on FHIR works, even if the systems you use today still feel disconnected.
Also Read: Generative AI in Healthcare: Top Applications and Use Cases
Before you think about how to develop SMART on FHIR apps, it is important to understand what actually sits underneath it and why these pieces exist at all. Healthcare systems did not begin with interoperability in mind, and they were built in parts, and over time, and therefore the data ended up scattered across tools and platforms. FHIR, interoperability, SMART, and OAuth 2.0 were created because of that problem but also because healthcare needed a safer way to share information and a more predictable one too… so that things could finally connect.
FHIR stands for Fast Healthcare Interoperability Resources and it is a standard that defines how healthcare data should be structured and shared. It tells systems how to describe things like
so that different platforms can understand the same data in the same way, even when those platforms were built by different vendors and for different purposes.
Before FHIR existed, many healthcare systems used their own formats and because of that, moving data from one system to another often required custom logic. It was slow, it was fragile, and it usually broke when one system changed. With FHIR, data is exposed through APIs and those APIs follow a common model so that applications can request information without guessing how it was stored or where it came from.
This matters in healthcare because clinical decisions depend on accurate and timely data. And when information is delayed or when it cannot be accessed easily, care teams work with only part of the picture and sometimes that is not enough. FHIR was created so that data could move more freely, but also so that it could remain structured and controlled and secure at the same time.
Healthcare interoperability is the ability of different systems to exchange data and then to actually use that data in a meaningful way. It is about making sure the receiving system understands what the data means and how it should be used.
In many real environments, hospitals use multiple platforms at the same time, such as
These systems may all store information about the same patient, but they do not always stay aligned, and therefore gaps appear. So when a clinician looks for context, the data may exist, but it is spread across tools that do not fully connect… and the work becomes harder than it should be.
Interoperability exists to reduce duplication and confusion and manual effort as well, but it also creates new technical and security challenges because once data can move more easily, it must also be protected more carefully, and that balance is not always simple or smooth.
SMART is a framework. It defines how third-party applications can safely run inside healthcare systems and focuses on how an app launches and how it identifies a user and how it requests permission to access specific data. In easy terms, SMART controls how an app enters the clinical environment and how it behaves once it is there which matters more than it sounds.
OAuth 2.0 is the authorization protocol that SMART relies on, and it manages how access tokens are issued and how permissions are granted. Instead of giving an app full access to a system, OAuth 2.0 allows access to be limited to
Together, SMART and OAuth 2.0 make it possible for healthcare apps to connect to sensitive systems without exposing credentials or bypassing security rules. This is important because healthcare data is regulated, and because patient information cannot be treated like general application data. Security is not optional here… and it never really was.

SMART on FHIR brings these ideas together. It combines the data model of FHIR with the access and security framework of SMART and OAuth 2.0. So instead of only defining how data looks, it also defines
An application can launch inside an EHR, can request permission to access certain FHIR resources and then retrieve or update data through standardized APIs with SMART on FHIR. And this happens without breaking existing workflows and without forcing providers to rebuild their systems again and again, which is the part that usually matters most.
In practice, this means developers can build apps that work across different EHR platforms, as long as those platforms support SMART on FHIR. It also means hospitals can adopt new tools without rewriting integration logic each time. The foundation is shared, and therefore the risk is lower, and the behavior is more predictable, even if the use cases themselves are very different… and sometimes still evolving.
When teams talk about healthcare app development today, they are not only talking about screens and features, but also about the data, and the access, and the security, and how information moves between systems so that clinical workflows do not break. This is where people start talking about how to develop SMART on FHIR apps, because this matters as it sits between the application and the Electronic Health Record (EHR) system, and it controls how the two connect, and how they continue to talk to each other.
In simple terms, SMART on FHIR works like a bridge. The app connects to an EHR by using a FHIR API for apps, and then SMART manages how the app is launched and how permissions are granted. So instead of pulling data in unsafe or unclear ways, the app follows a defined path. It asks for access, and it receives a token, and it only sees the data it is allowed to see, therefore the flow stays controlled… even when systems are complex.
From a development point of view, this changes how FHIR app development has been handled in the past. Developers were forced to build custom integrations for every EHR vendor, but now they can design one flow that works across systems that support SMART on FHIR. This reduces dependency on vendor-specific logic, and therefore reduces long-term maintenance effort, which matters in healthcare more than it first appears.
SMART on FHIR also supports modern use cases, such as
These tools need access to real-time data, but they also need to stay inside existing workflows. SMART on FHIR allows an app to launch directly within an EHR session, so that clinicians do not need to leave their system to use it. The data appears where the work already happens, and because of that, adoption becomes easier… even if the technology behind it is not simple.
Compliance is another reason this model matters. Healthcare data cannot be handled casually, and systems must follow strict rules. By using standardized authorization and defined data scopes, SMART on FHIR supports HIPAA-compliant healthcare app development without forcing teams to design security models from scratch. Security becomes part of the connection itself, and not something added later.
From a business perspective, SMART on FHIR app development also affects cost and scalability. When apps are built on a shared standard, they can be reused across hospitals instead of being rebuilt each time. This influences the cost to build healthcare app solutions, because integration time is reduced, and testing becomes more predictable over time.
So when organizations think about how to develop SMART on FHIR apps, they are not only choosing a technical approach. They are shaping how data flows, and how systems remain compliant, and how future tools will connect to their EHR environment. In that sense, SMART on FHIR becomes part of the foundation of modern healthcare app development, even if users never see it directly… and even if they do not always realize it.
When people ask how to develop SMART on FHIR apps, they often expect a short checklist, but in real healthcare app development, the process is not only technical. It is also about understanding the use case, and the data, and the security rules, because the app will connect with Electronic Health Record (EHR) systems. SMART on FHIR app development therefore starts with planning, and not only with code… even though code matters later.
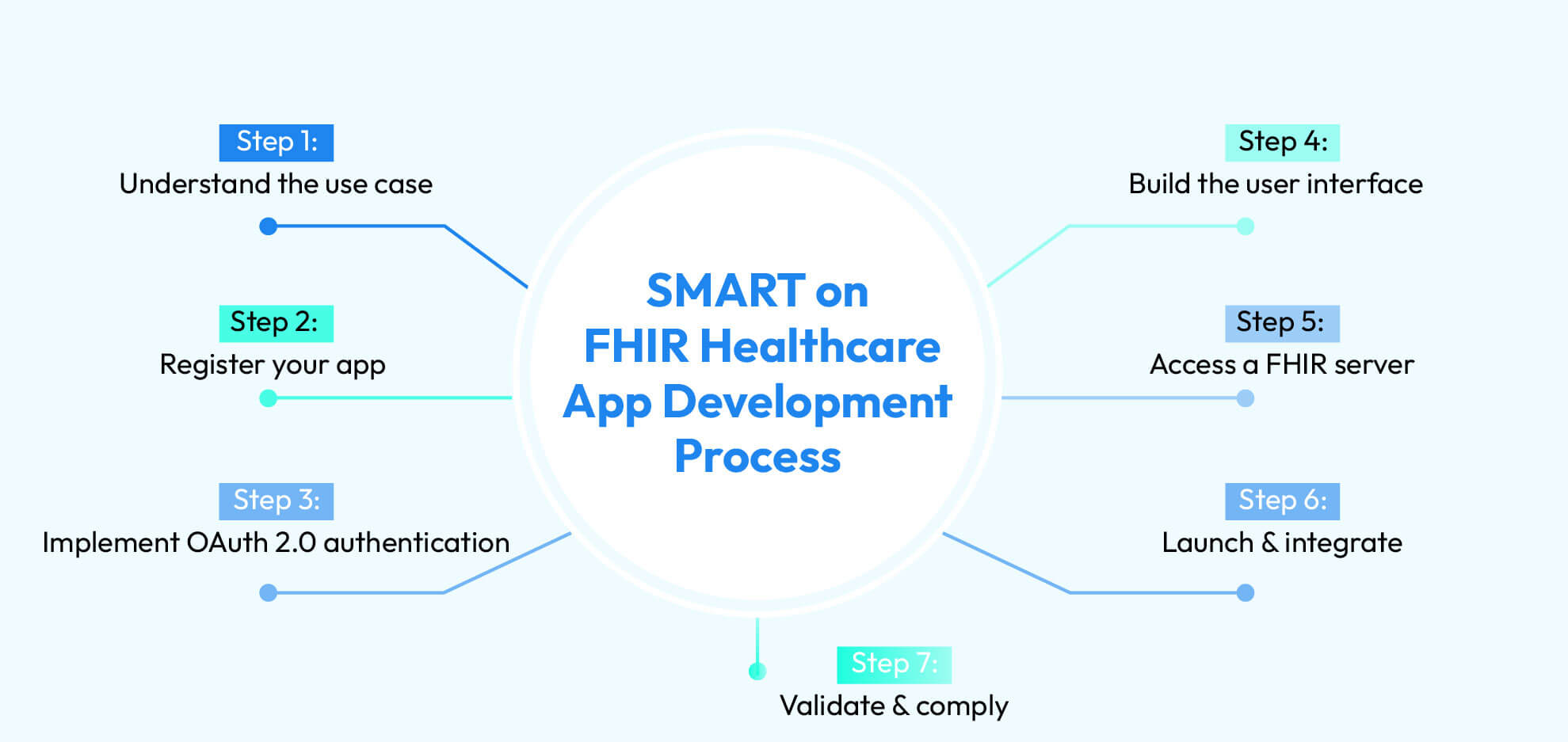
First you need to define what the app is supposed to do and who it is built for before you write any logic because some apps support clinicians, some support patients and others focus on analytics or coordination. So the use case decides which FHIR resources are required and how the data will be used.
At this stage, teams usually decide:
This step matters because it shapes the scope of SMART on FHIR integration, and therefore it also affects the cost to build SMART on FHIR app solutions later… even if that is not obvious at first.
Once the use case is clear, the app must be registered with the target EHR system or FHIR server. Because registration will let the system recognize the app and decide how it can connect. During this process, the app receives a client ID and redirect URLs.
This is where FHIR app development becomes real, because you are no longer working only with test logic. You are preparing the app to interact with live healthcare systems, but still in a controlled way, so that access stays limited.
Authentication is not optional in healthcare, and SMART on FHIR relies on OAuth 2.0 for that reason. OAuth 2.0 manages how users log in and how permissions are granted, so that the app does not receive full access by default.
At this step, developers configure:
This is how SMART on FHIR app development supports HIPAA-compliant healthcare app development, because access is controlled, and data is protected, and nothing is exposed by accident.
With authentication in place, attention moves to the user interface, because this is the part people actually see. In healthcare app development, the UI must be simple, but it must also handle structured data coming from EHR systems.
Design choices depend on the use case. A patient app may focus on clarity and summaries, but a clinical tool may focus on speed and depth. In both cases, the interface must work with FHIR data models, and not against them, because the app depends on that structure.
At this point, the app connects to a FHIR server using a FHIR API for apps. This is how it retrieves patient records, observations, medications, and other resources.
Instead of hardcoding logic, the app requests standardized FHIR resources. This allows the same application to work across different systems that support SMART on FHIR integration. It also reduces long-term maintenance effort, because one change in an EHR does not always mean one change in the app… which saves time later.
After the main features are built, the app is launched inside the EHR environment or connected to the healthcare system. This is where integration becomes visible. The app must open in the right context, receive patient or user information, and return outputs without breaking workflows.
This step usually includes:
It is also the moment when teams start to see how SMART on FHIR app development behaves outside a test setup, and inside real environments.
Validation and compliance is the final step. Healthcare data is regulated and apps must meet security and privacy rules before real use. Testing focuses not only on features, but also on access control, data handling, and audit behavior.
This step is critical for:
Without this layer, even a well-built app can fail in production… which is something teams usually discover too late.
Overall, how to develop SMART on FHIR apps is not just about connecting to a FHIR server. It is about designing around standards, and workflows, and compliance at the same time. When it is done correctly, SMART on FHIR app development creates healthcare apps that are easier to integrate, easier to scale, and more aligned with modern EHR systems.
And because of that, both the development effort and the cost to build healthcare app solutions become more predictable over time… which is something healthcare teams care about more than they first say.
Also Read: Healthcare Chatbot Like Google’s AMIE: Features, Benefits, and Development Cost Explained
When you step into healthcare app development, and you decide to work with SMART on FHIR, the way the app is planned and the way it connects with systems are different. It is not just about building another health app, but about building something that can live inside EHR systems, and because of that, it must care about interoperability and security and also about usability. Therefore, SMART on FHIR app development has been shaped more around data access than data storage, so that the right information can be shown at the right time, but also in the right format.
At the base level, these healthcare apps are built on Fast Healthcare Interoperability Resources, and the patient data was kept in a structured form, so that it can move between systems, and it does not lose meaning while moving. This is why SMART on FHIR healthcare apps are usually chosen when long-term system connection is required.
These apps are designed so that they can sit inside existing EHR systems, and users do not have to leave their main screen. It helps because workflows stay connected, but also because clinicians do not waste time switching tools.
Data is exchanged through controlled access layers, and only approved users can see it. Workflow hooks for refills, billing, and prior authorizations are added, therefore medical practice becomes more automated, but not complicated.
Because FHIR standards are used, the app can work with many EHR and EMR systems, and not just one vendor. This makes healthcare interoperability easier, and also more realistic for growing systems.
SMART on FHIR relies on OAuth 2.0 and identity verification methods, so users are checked before data is opened. This means patient data is protected, and healthcare app development stays aligned with compliance needs, even if systems change.
Users log in once, and then they can move between connected health apps and clinical tools. It sounds simple, but it removes repeated logins, and therefore improves daily usability.
These apps were designed to reduce paperwork and screen overload, so healthcare professionals can focus on care instead of navigation, which is still a problem in many systems.
They connect easily with pharmacy tools, lab systems, and care platforms, so that the app does not work alone, but works as part of the larger healthcare software ecosystem.
Since they follow open standards, these apps can be updated and connected with new digital health tools later, therefore long-term system growth becomes easier.
The app UI appears within the EHR screen, so users do not need to open external windows. It feels like part of the system, and not like an added layer.
Data exchanged between the app and the EHR remains accurate and protected, so that records do not mismatch, and trust in the system stays stable.
SMART on FHIR supports web apps, mobile health apps, and cloud-based healthcare systems, therefore developers are not locked into one structure.
Cloud deployment improves scalability and access, and it allows healthcare apps to be used across locations, but with controlled security settings.
Taken together, these features explain how SMART on FHIR app development usually works. You begin with secure interoperability, and then you add EHR integration, and after that, you build for scale, so that the healthcare system can grow without rebuilding everything again. It is not fast always, but it is more stable over time.
SMART on FHIR features are used across many healthcare scenarios, and not only in hospitals, but also in research and patient care systems.
These apps support teams in cancer care, memory care, hospice care, and chronic treatment programs, because communication and task tracking are kept in one place.
They help manage study data, and participant surveys, and trial progress, so that real-time data can be captured and reviewed.
Patient information is converted into charts and dashboards, so patterns become easier to read, and decisions are not based only on raw records.
Apps support diabetes, heart disease, respiratory issues, cancer, and mental health conditions, by tracking symptoms and daily health changes.
Some apps use genetic or behavioral data along with clinical data, so recommendations are more specific, but still grounded in medical records.
Reminders and progress tracking help patients stay on schedule, therefore treatment plans are followed more closely.
These apps allow messaging and remote consultations, and patients can access their records, so involvement in care decisions increases.
Large sets of data are reviewed to identify disease patterns, so that public health strategies can be planned more carefully.
Health records are used to calculate possible future risks, such as diabetes or heart disease, and this helps with early intervention.
Vaccination history and health documents can be stored and organized, so that travel and personal care planning becomes easier.
When organisations start deciding on how to develop SMART on FHIR apps for their business, they take one step towards improving interoperability and security, and also prepare for scalable digital health systems.
These apps do not only store data, but they support how care is delivered, which is why SMART on FHIR in health app development has been growing slowly, and steadily, even when system change feels complex.
SMART on FHIR apps are built because healthcare systems need to share data, and they also need to protect it, so the benefits are not only technical, but also practical. It is about how the app connects, and how the data moves, but also about how people actually use it in daily healthcare work. Therefore, SMART on FHIR app development has been seen as useful not just for developers, but for hospitals and patients too… in different ways.
Along with understanding how to develop SMART on FHIR apps, it is also important to know their benefits for hospitals as well as patients.

For hospitals, SMART on FHIR apps change how healthcare app development connects with EHR systems, because the apps can live inside existing workflows, and still follow FHIR standards, so that integration does not feel forced.
Patient data can move between EHR apps and healthcare platforms, and therefore information is no longer locked inside one system, but shared when it is needed.
Doctors and staff access the same data inside their usual tools, so time is saved, but also errors are reduced, because systems are finally aligned.
With OAuth 2.0 and controlled authorization layers, hospitals can support HIPAA-compliant healthcare app development, and patient records are protected, even when multiple apps are connected.
Instead of building custom links for every system, SMART on FHIR integration offers a standard method, therefore long-term development and support become easier.
Hospitals can connect AI in healthcare apps, analytics platforms, and clinical decision tools to EHR data, which was difficult when systems were closed.
For patients, the benefits appear in access and continuity, because their health data can follow them across systems, and not stay tied to only one provider.
Patients can view their information through connected EHR apps and healthcare platforms, and it feels more transparent, but also more reliable.
When doctors use the same standardized data, treatment plans stay connected, therefore gaps in care are reduced, but communication also improves.
Authorization rules make sure only approved users and apps can access medical data, so patient trust is maintained, even when more tools are added.
Apps combine FHIR API for apps with analytics and AI, so insights are based on real patient data, and not just general assumptions.
Patients move between apps without repeated logins, and their data remains consistent, which makes digital healthcare easier to use, even though the systems behind it are complex.
Now that we understand how to develop SMART on FHIR apps, their features, and benefits also. It’s the time to know the cost of SMART on FHIR app development because it is not the same for every project, as the app can be small or complex, and it can connect with one system or many systems, and therefore the budget changes with the scope. When you look at the cost to build a SMART on FHIR app, it is usually explained as a range, and not as one exact number, because the features and compliance needs are different every time.
In general, a basic SMART on FHIR healthcare app can start around $25,000 to $40,000, but if the app includes advanced workflows, and deeper SMART on FHIR integration, or AI in healthcare app features, the cost can move toward $70,000 or more. It depends on what the app does, and how much data it touches, and also how secure it must be… so pricing shifts.
Some main factors that affect the cost are:
So, the cost to build a healthcare app using SMART on FHIR is shaped by how much data you move, and how safely you move it, and how many systems you connect to. It is not only about coding, but about security and long-term maintenance too, and that is where most of the cost usually sits… even if it is not always visible at the start.
As a trusted healthcare app development company, Techugo helps businesses wondering ‘how to develop SMART on FHIR apps’ because the process is not only about coding, but also about how the app connects with EHR systems, and how the data is handled, so that everything stays secure and usable at the same time. It works with healthcare app development needs first, and then with SMART on FHIR integration, therefore the app is shaped around real clinical use, but not just around theory…
The team builds apps using FHIR API for apps and secure authorization, so data access is controlled, and workflows are protected, but still flexible for growth.
As a leading mobile app development company for healthcare mobile applications, Techugo brings development and compliance together, so the cost to build a SMART on FHIR app becomes easier to plan, and the final product is more stable for real healthcare environments… even when systems are complex.
If you’re also thinking about how to develop SMART on FHIR apps, then contact us today. We’re ready to become your partner.
FHIR is the standard that defines how healthcare data is structured and shared, and it explains what the data should look like, but SMART on FHIR explains how apps can safely use that data. So FHIR focuses on the format, and SMART focuses on access, and because of that, they work together, but they are not the same thing. You can say FHIR was made for data exchange, and SMART on FHIR was made for app connection, therefore both are needed when you build modern healthcare apps.
SMART on FHIR apps work with EHR systems by using FHIR APIs and OAuth 2.0, so the app first asks for permission, and then the EHR system decides if access should be given or not. Because of this process, the app can read patient data, and sometimes write data back, but only after it is approved. It runs inside or beside the EHR workflow, therefore users do not need to leave their system, and data is shared without breaking existing processes…
Yes, SMART on FHIR is secure for healthcare app development, because it uses authorization layers like OAuth 2.0 and OpenID Connect, so that only approved users and apps can see patient data. When these security methods are combined with encryption and proper compliance practices, it supports HIPAA-compliant healthcare app development, and patient information stays protected. It is not only about access, but about control, and because of that, trust in the system is maintained.
Write Us
sales@techugo.comOr fill this form