Write Us
We are just a call away
[ LET’S TALK AI ]
X
Discover AI-
Powered Solutions
Get ready to explore cutting-edge AI technologies that can transform your workflow!


Every single day, healthcare companies submit millions of both insurance claims and accounts receivable (A/R) claims. However, when it comes to claims denials, nothing is routine, as the delay in receiving payment from these denials can slow down revenue timing, create additional administrative burden throughout the organization, and lead to lost revenues if the denials are not properly managed. Herein lies the power of implementing a denial management automation system.
Denial management automation refers to the use of software and intelligent workflows to identify, track, analyze, and resolve denied claims. This focuses on automatic denials or with little human intervention. Rather than having to manually examine every single denied claim, the use of automation tools will allow you to:
The aim is to decrease the number of overall denials, resolve them more efficiently, and eliminate the occurrence of these claims being denied in the future.

When implementing a new technology like denial management, it is worthwhile to consider the reasons how it can affect your business. So, some of the reasons for hospital denial management solutions include:
When dealing with a manual workflow, there will be a person assigned to complete every one of these 6 tasks when dealing with denied claims:
For each of those 6 tasks, depending on how busy the team is, it could take anywhere from a few minutes to several days to complete per claim.
Through the help of automation, the process reduces:
When using an automated process, claims will be able to be processed without being in a queue at a very fast rate. High-priority claim denials (based on value) can be handled first automatically.
Many mistakes can happen during the handling of manual claims denials (for example, experienced staff can interpret denial codes incorrectly, enter incorrect data, miss required documents, and apply inaccurate corrections). As a result of these errors, claims denials will occur again, increasing workload and delaying payment.
Fewer resubmissions due to erroneous denials will lead to a reduction in duplicated work and provide more consistent outcomes for the industry.
An enormous challenge in denial management is that not all denied claims are followed up on. This is often due to limited staff and time; therefore, some claims are prioritized while others go unattended.
With automation in place to ensure each denied claim is addressed by:
Finding patterns and trends throughout the many different manual denial management processes is too much effort for one person. The data is distributed across many different spreadsheets, systems, and the person’s ability to remember.
Automation tools typically have built-in analytic and reporting capabilities that:
The automation will make it considerably easier to identify trends such as:

If you expect that revenue cycle denial management automation, RCM denial management automation, or any other form is a one-time process, then you might have to re-evaluate. Shaped by the maturity in the revenue cycle, healthcare denial management automation happens in multiple stages. Thus, to understand it better, one needs to go through the stages, which consist of:
You have to know how to handle denials before implementing a new system. How will you keep track of the denials you receive and work through them until they are resolved? You must also know who is working on them, how they are tracked, and how long it takes to resolve denials on average. You may be able to determine patterns, such as the most common denial reason, high-risk payers, and workflow bottlenecks, by looking at historical data from the previous few months.
Once you know how you currently process denials, the next step is to structure your denial data. Proper categorization of denials is essential so that automation can be based on consistent and standardized input. If the reason for a denial is inconsistent or not clearly defined, then automation tools will not work correctly and will not have the ability to assign workflows to denials or to apply rules to those denials.
Deciding on the right automation tool can greatly affect the success of your automation projects. While some may want to focus on advanced features, it is really more important to pick a solution that fits your company’s unique needs and challenges. For example, if your wish is to have it done quickly and as efficiently as possible, then focus on workflow automation features. Hence, it is a crucial aspect of medical billing denial management automation.
Also Read – Top 10 Best AI Tools for Coding in 2026
After determining your automation tool, it is now time to integrate it into your existing systems, including your EHR, PMS, and billing solutions. If done correctly, the automated tool will seamlessly allow the flow of data between systems without manual input and duplication of data. The ability to capture and process denial-related information in real time will provide an improvement in efficiency and accuracy.
Once the integrations have been completed, you can start creating automated workflows that help to determine how to process and resolve different types of denials. A workflow is a sequence of activities that your system will take when it receives a denial, and there are some denials that can even be automatically corrected and resubmitted.
The denial rules engine is the component of your automated processes that makes the decisions about how to process and resolve each of the denials that it receives according to the criteria defined in the pre-existing rules. The Denial Rule Engine can use a variety of criteria to establish how to process and resolve each denial, including the dollar amount associated with the claim, the type of denial, and whether the denial contains an error or not.
Insights derived from the system can also help you to know how to resolve recurring issues. They can reveal if there are any common patterns increasing denials. For example, eligibility issues caused by incorrect information being entered into the front desk, or recurring claims that were denied due to improper coding. By addressing these underlying causes of denials, you will prevent the same issues from happening again and increase efficiency.
You must keep an eye on your key performance indicators, including but not limited to denial rates, resolution times, and recovery rates. This will allow the employee (your entire RCM team) to see what areas of their workload are performing well, what areas need improvement, as well as how to spot new problems and adjust workflow when necessary. Dashboards and regular reports make it much easier for you, the employee, and the rest of your team to monitor performance and share findings regularly.
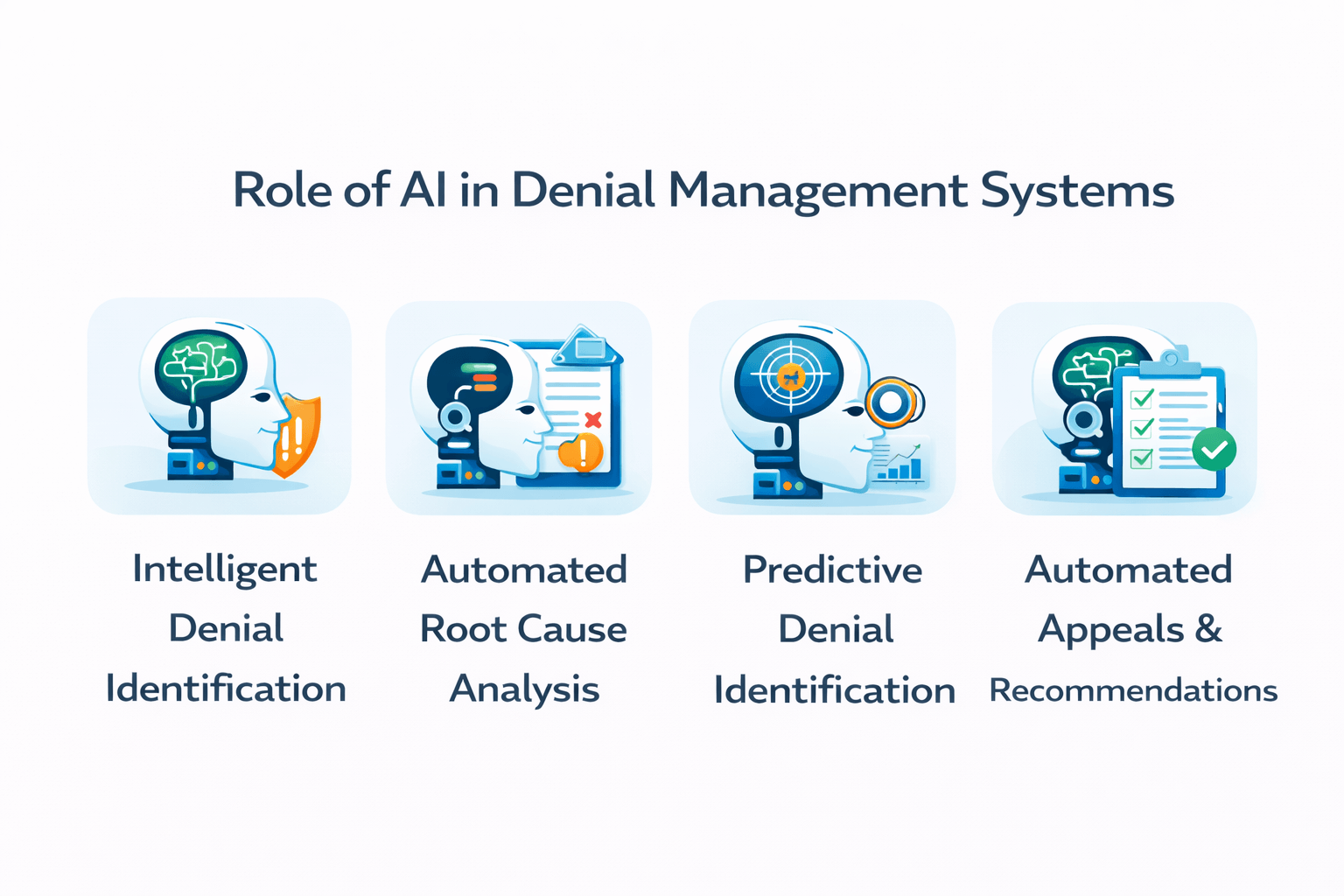
Managing cost, reducing administrative burden, and enhancing revenue have become the aims of businesses in almost every domain. Therefore, to tackle this, artificial intelligence is emerging as the go-to tool. Thus, the role of AI in denial management systems includes:
AI’s initial function is to determine which claims have been denied and to uncover the reasons for their denial in a very efficient way.
Because traditional systems require users to read payer responses manually and decode the codes within them, this process takes a lot longer and can be confusing at times. AI reduces the time and complexity of this process by automatically reading denial messages, extracting important pieces of information, and categorizing the reason for denial.
AI can be used in ways such as:
AI doesn’t stop at just identifying denied claims. It can also analyze patterns and trends to determine the root cause of denials. Instead of asking “What was wrong with this claim?” AI answers the question “Why does this keep happening?” Moreover, AI can help you find:
Artificial intelligence can be used to analyze historical data and provide insight into claims that may be denied prior to submitting them. This gives teams the opportunity to take action before it is too late. This is how it functions:
With AI, automation is improved as workflows will be more intelligent and adaptable. Whereas a fixed rule-based workflow would have existed, AI can:
If you look at the resume of Techugo, you will come across a range of advantages that you can use in your denial management automation software:
Therefore, if you are looking to automate the medical billing cycle, want to get that outstanding accounts receivable, and enhance your overall revenue, then Techugo is the way to go. So, get in contact with one of the best mobile app development company in USA, now
The process of denial management automation changes how efficiently the healthcare revenue cycle operates. This includes identifying, sorting, and resolving denied claims with as little manual intervention as possible. In addition to speeding up the process and reducing the risk of human error, it increases revenue recovery while providing actionable information through analytical capabilities and AI functions. Hence, in the Middle East market, it is crucial to seek help from a healthcare app development company like Techugo.
Ans) Yes, many solutions are designed for small and mid-sized practices that are easy to implement.
Ans) Providing insights to prevent constant issues, standardizing processes, and identifying errors early does help in minimizing denials.
Ans) The best mobile app development company in India is Techugo. With 10+ years of experience helping mature and nascent-stage startups, we have built the track for success in entrepreneurship.
Write Us
sales@techugo.comOr fill this form